Ulcers: What You Need to Know Right Now
Got a burning pain in your stomach or a sore that won't heal? Ulcers are common and they range from mouth sores to deep peptic ulcers in the stomach or duodenum. Most people worry first about pain and bleeding — and that’s smart. Recognizing symptoms and getting the right tests speeds up relief and keeps small problems from becoming emergencies.
How ulcers start (plain language)
Peptic ulcers happen when the protective lining of the stomach or small intestine breaks down. The two usual culprits are Helicobacter pylori (H. pylori) infection and regular use of NSAIDs like ibuprofen or naproxen. Smoking and heavy alcohol make healing slower. Mouth ulcers can follow minor injuries, tension, or low levels of certain B vitamins. Pressure ulcers appear from prolonged pressure on skin in people who can't move well.
Here’s what that means for you: if you take NSAIDs often or have a history of heartburn, your risk goes up. If you have ongoing mouth sores or non-healing wounds, mention it to your clinician — it could be a sign of an underlying issue.
Common signs, tests, and quick treatments
Signs to watch for: a burning or gnawing pain (often between meals), bloating, heartburn, nausea, unexplained weight loss, black or tarry stools, or vomiting blood. Mouth ulcers are usually small, painful, and white or yellow with a red border. Pressure ulcers start as red patches and can deepen if not relieved.
How doctors check: a breath or stool test for H. pylori, blood tests, and sometimes an upper endoscopy to look directly at the lining. For pressure ulcers, clinicians check how long someone’s been immobile and examine skin layers.
Treatment basics you can expect: if H. pylori is found, a short course of antibiotics plus a proton pump inhibitor (PPI) usually clears it. If NSAIDs caused the ulcer, stopping or switching meds and using a PPI helps healing. Antacids, H2 blockers, sucralfate, and topical gels (for mouth ulcers) can ease symptoms. Pressure ulcers need pressure relief, proper wound care, and sometimes antibiotics if infected.
Practical tips that actually help: stop NSAIDs when possible or take them with food and the lowest effective dose; avoid smoking and cut back on alcohol; start PPIs as your doctor advises (often before a meal); don’t skip the full antibiotic course if treating H. pylori; and protect at-risk skin with regular repositioning and moisture management.
See a doctor right away if you have severe, sudden stomach pain, vomiting blood, black stools, fainting, or a large non-healing wound. Those are red flags that need urgent care.
Want more? Check our related articles for deeper guides on H. pylori testing, safe painkiller choices, and wound care basics to help manage ulcers safely at home and avoid repeat episodes.
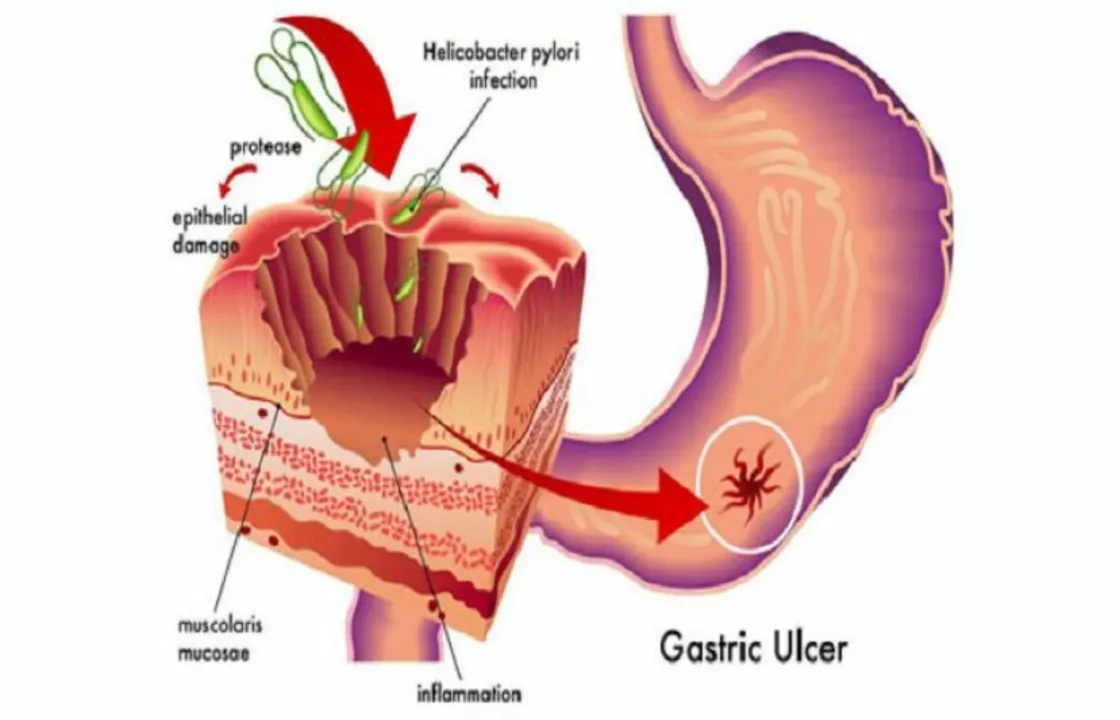
The link between ulcers and Helicobacter pylori infection
I recently came across some fascinating information about the link between ulcers and a bacterial infection called Helicobacter pylori. It turns out that the majority of ulcers are actually caused by this bacterium, and not by stress or spicy foods, as was once believed. H. pylori infections can be treated with antibiotics, which can ultimately lead to the healing of ulcers. This discovery has truly revolutionized the way we approach and treat ulcers. I'm glad I stumbled upon this, and I hope it helps others better understand the real cause of ulcers.
More Detail