Barrett's Esophagus — What You Need to Know Right Now
Ever had heartburn so bad it felt like it would never end? If that reflux lasts for years, it can change the lining of your lower esophagus. That change is called Barrett's esophagus. Most people with Barrett’s won't get cancer, but it raises the risk enough that doctors want to watch it closely.
How Barrett's esophagus is diagnosed
Barrett's often shows up during an endoscopy done for long-term GERD (gastroesophageal reflux disease). During the procedure a doctor looks at your esophagus and takes small biopsies. The lab checks those samples for abnormal cells and classifies them as no dysplasia, low-grade dysplasia, or high-grade dysplasia. That label determines what happens next.
Don’t rely only on symptoms: some people with Barrett's have mild or no heartburn. If you have chronic reflux, a history of smoking, obesity, or you’re an older white male, mention Barrett's to your doctor — you might need an endoscopy.
Treatment and follow-up
Treatment has two goals: control acid and prevent progression to cancer. Proton pump inhibitors (PPIs) are the main medicine to reduce stomach acid. For people with dysplasia, endoscopic treatments like radiofrequency ablation (RFA) or endoscopic mucosal resection (EMR) remove abnormal tissue and cut cancer risk.
Surveillance schedules depend on biopsy results. Typical plans are: no dysplasia — endoscopy every 3–5 years; low-grade dysplasia — repeat every 6–12 months or consider ablation; high-grade dysplasia — immediate endoscopic therapy is usually recommended. Your gastroenterologist will tailor the plan to your age, health, and biopsy findings.
Simple lifestyle moves help too. Lose excess weight, quit smoking, limit alcohol, raise the head of your bed, and avoid meals close to bedtime. These steps won’t cure Barrett’s but they reduce reflux, which helps protect the esophagus.
What to expect during an endoscopy: you’ll get light sedation, the scope is passed gently into the throat, biopsies are quick, and most people go home the same day. Recovery is usually fast — you might have a sore throat for a day or two.
Watch for warning signs and call your doctor if you get new trouble swallowing, painful swallowing, unexplained weight loss, vomiting blood, or persistent chest pain. Those symptoms need prompt attention.
If you have Barrett's, keep regular follow-up and ask questions: How often should I be scoped? Is ablation right for me? What lifestyle changes matter most? Clear answers help you avoid surprises and lower your long-term risk.
Want to read more patient-friendly guides or check specific treatments? Our site has easy articles on GERD, endoscopy, and endoscopic therapies to help you feel informed and in control.
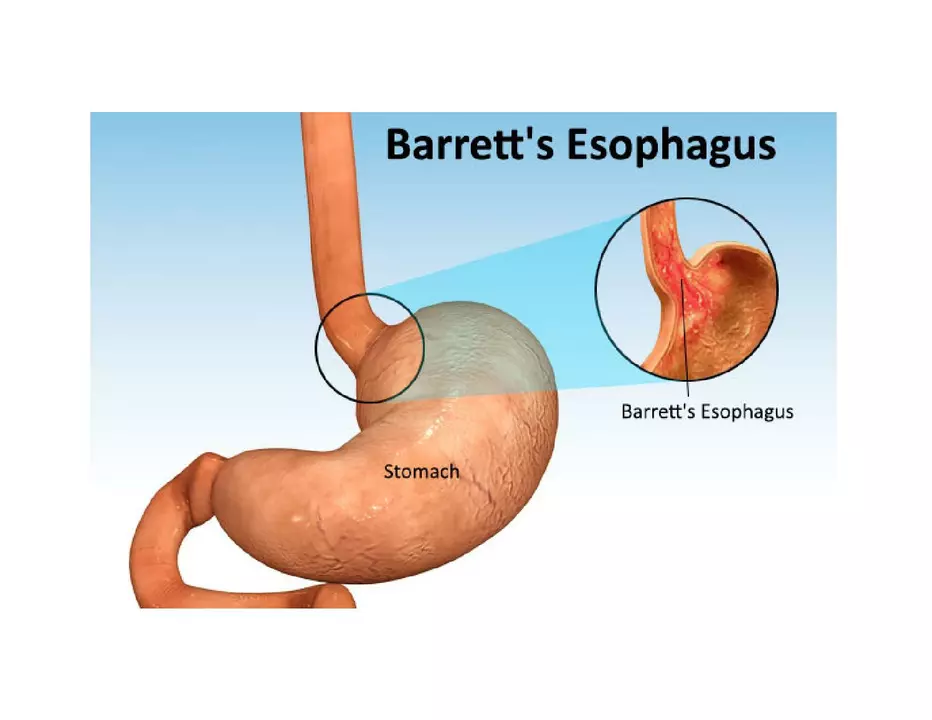
The effectiveness of Lansoprazole for treating Barrett's esophagus
I recently came across some interesting information about the effectiveness of Lansoprazole in treating Barrett's esophagus. It appears that this medication, which belongs to the proton pump inhibitor (PPI) family, can significantly reduce the production of stomach acid and alleviate symptoms associated with Barrett's esophagus. Moreover, Lansoprazole has shown promising results in preventing the progression of this condition to esophageal cancer. However, it is important to remember that while Lansoprazole can be an effective treatment option, it may not work for everyone and should be taken under the guidance of a medical professional. Overall, it's fascinating to learn about the potential benefits of this medication in managing Barrett's esophagus and improving the quality of life for those affected.
More Detail